Blog
At What Bilirubin Level is Phototherapy Required

When you are given the information that your baby has jaundice, it is overwhelming. As a parent, you will tend to question yourself on the extent and actions that you need to take. The big questions that come to mind include at which bilirubin level is phototherapy required? It is a normal concern and you are not alone who feels slightly confused as to what to do next.
All the details you need to know about bilirubin levels and when we need to use phototherapy will be broken down in this blog. We will explain this to you easily and provide useful tips to make the process easier. By the conclusion of it, you will already have an idea of what to watch out and how your little one can be helped with phototherapy.
At What Bilirubin Level is Phototherapy Required? (Complete Guide for Parents & Doctors)
Many babies are born with jaundice, as a result of high bilirubin levels. This may be alarming to parents and one would like to know at what bilirubin level is phototherapy required. Phototherapy aids in the reduction of bilirubin and prevents the occurrence of such complications as bilirubin induced brain damage.
When a baby requires phototherapy, it is important to know when the bilirubin level is phototherapy. In this guide, we shall address the bilirubin level at which phototherapy should be used and the use of total serum bilirubin (TSB) in gauging the severity of jaundice.
Phototherapy Threshold for Neonatal Jaundice Explained
The bilirubin level where phototherapy is required will differ according to the age of the baby, in hours and gestational age. In infants, phototherapy is generally thought to be used whenever the total serum bilirubin (TSB) rises to above 15 mg/dL in the case of a full term baby. In preterm babies, however, a lower cut off is used because they are more susceptible to bilirubin toxicity.
Overall, phototherapy is administered using the bilirubin threshold in order to avoid kernicterus and other complications related to neurological neurotoxicity of bilirubin. The assessment of jaundice severity is carried out frequently to provide an opportunity to intervene in time based on whether the bilirubin level requires phototherapy.
Total Serum Bilirubin (TSB) and Its Role in Treatment
The test that is mostly relevant to determine if the bilirubin level is phototherapy in a newborn is the total serum bilirubin (TSB). It assists medical workers in ascertaining whether phototherapy or other therapies are necessary. The greater the TSB level, the greater the amount of indirect hyperbilirubinemia, or buildup of bilirubin in the bloodstream, that the baby has.
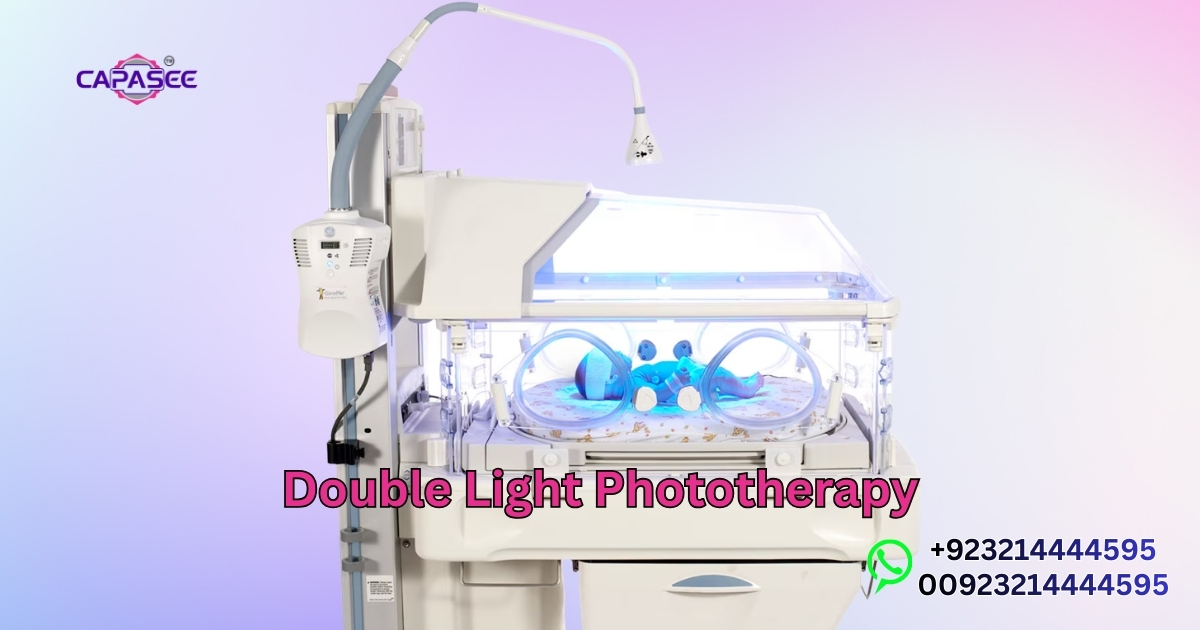
TSB measurement plays an essential role in the monitoring of serum bilirubin and the decision on the need to continue invasive therapy, such as exchange transfusion. The most widespread is blue light phototherapy, in which bilirubin in the skin of the baby is broken down.
Bilirubin Levels in mg/dL in Newborns: What’s Normal and What’s Risky
Normal bilirubin levels are normally below 12mg/dL in a baby. But anything beyond this may be a danger, particularly when it runs high in a short period of time. Infants with risk factors (such as hemolytic disease or deficiency of G6PD) and premature infants have a greater risk of high levels of bilirubin.
Elevated bilirubin levels may result in such severe illnesses as kernicterus, which is a form of brain damage. Doctors should pay close attention to whether the bilirubin level is phototherapy and initiate treatment when the levels are not too dangerous.
You May Also Read This Blog: Will Jaundice Reduce After Phototherapy
Phototherapy Guidelines in Pakistan for Newborn Jaundice

Phototherapy guidelines in Pakistan are adhered to according to international standards, yet are also adapted to local circumstances. These are the rules that assist physicians in evaluating whether the bilirubin level is phototherapy, considering the age of gestation and the health of the baby as a whole.
Such clinical jaundice guidelines indicate that blue light phototherapy is best suited to treat neonatal hyperbilirubinemia. Close checking of the bilirubin clearance rate must be regularly carried out to make changes in treatment.
National and International Bilirubin Phototherapy Guidelines Compared
In Pakistan, bilirubin phototherapy is mostly in line with the international standards. Nevertheless, there are certain local changes to consider in alternative healthcare environments and resource access. The aim is also the same to ensure timely intervention and determine when the bilirubin level is phototherapy to avoid bilirubin neurotoxicity.
International guidelines are concerned with early intervention with special emphasis on phototherapy initiation criteria and the necessity of prophylactic or preventive phototherapy in high risk newborns. These methods assist in reducing errors in serum bilirubin measurements and avoiding unnecessary medication.
Treatment Guidelines for Newborn Jaundice in Pakistan
In Pakistan, treatment guidelines emphasize bilirubin in all newborns, particularly those who are at high risk. In full term babies, phototherapy is often initiated with a TSB level that is above the normal level of 15 mg/dL, which helps determine when the bilirubin level is phototherapy required.
In the case of preterm babies, the limits are set lower and treatment commences even with lower bilirubin levels to avoid permanent harm. Medical workers also check the level of albumin and jaundice and make sure that the bilirubin clearance rate is the best to recover.
Serum Bilirubin Measurement Methods (TSB vs TcB Accuracy)
Serum bilirubin can be measured in two ways, total serum bilirubin (TSB) and transcutaneous bilirubin (TcB). TSB is less invasive and can be implemented in early screening, but TcB is more precise and it needs samples of blood.
The two approaches are not mutually exclusive, but the gold standard of determining if bilirubin level is phototherapy is TSB. TcB can give prompt results, yet in some cases might not be considered very reliable in the evaluation of neonatal jaundice.
Phototherapy in Preterm vs Term Babies: When to Start Treatment
In case of a newborn that has jaundice, it should be assessed to determine the bilirubin level is phototherapy required. In the case of full term infants, phototherapy is normally initiated when the total serum bilirubin (TSB) levels attain a specific goal. Phototherapy can be required earlier in preterm infants whose liver is not completely evolved.
Phototherapy threshold is determined by the gestational period and age in hours postnatally. In premature babies, the complications can be caused even by lower levels of bilirubin, and blue light phototherapy might have to be implemented in earlier infancy.
Jaundice Phototherapy Indications for Full Term Infants
In full term infants, phototherapy has been advised when TSB exceeds the phototherapy threshold. This is typically approximately 15 mg/dL, though it is affected by such factors as bilirubin toxicity and age in hours. These are key parameters in assessing whether the bilirubin level requires phototherapy. Phototherapy is used to break down bilirubin so it does not accumulate and harm the brain of baby.
Phototherapy Guidelines for Premature Infants (Preterm Safety Levels)
Premature infants are more vulnerable to brain damage caused by bilirubin because their livers are not as efficient at handling bilirubin. In preterm infants, the lower limit of phototherapy is reduced and blue light phototherapy is commonly initiated at an even lower level in TSB of 10mg/dL. These recommendations are made specifically to assess when bilirubin levels require phototherapy and decrease the chance of kernicterus as a severe complication.
Exchange Transfusion Threshold and Critical Bilirubin Levels
In others, when the bilirubin level increases excessively, it can necessitate an exchange transfusion. This process is conducted when TSB levels are above the critical levels of bilirubin, which is normally above 20 mg/dL. Transfusion Exchange transfusion is useful in the urgent reduction of bilirubin and in the prevention of bilirubin neurotoxicity. It is a treatment of life threatening cases of neonatal hyperbilirubinemia, as a last resort.
Complications of High Bilirubin Levels in Babies if Left Untreated

When jaundice is untreated, bilirubin toxicity may cause severe injuries, including kernicterus, a brain injury of rare and severe severity. Other organs may also be impacted by high bilirubin levels and leading to long term neurological problems. That is why the importance of the early use of phototherapy is to avoid brain damage caused by bilirubin.
Kernicterus Risk and Dangerous Bilirubin Levels
Kernicterus is a devastating neurological disorder that is devastating and is due to high bilirubin levels in the brain. It happens when the bilirubin accumulates and influences the central nervous system. High bilirubin babies and neonatal hyperbilirubinemia cases run the risk of developing kernicterus unless phototherapy or other measures are administered.
Early Warning Signs That Indicate Urgent Phototherapy
Yellowing of skin and eyes is an early symptom of the need to use phototherapy and is a sign of the accumulation of bilirubin. The severity of jaundice analysis is required to discern the phototherapy initiation criteria. In case the bilirubin level of a baby increases too fast or beyond the reasonable limits, the early administration of phototherapy will help avoid irreversible harm and complications.
Management of Hyperbilirubinemia in Neonates Safely
Treatment and management of hyperbilirubinemia among the neonates involves close observation of the serum bilirubin. Severe cases might be subjected to neonatal intensive care, particularly preterm babies. High risk infants can also be given prophylactic or preventive phototherapy to prevent future problems facing the infant due to the brain damage caused by bilirubin. Medical teams must regularly evaluate if a bilirubin level is phototherapy to guide effective treatment.
Monitoring and Stopping Phototherapy Safely in Infants

In case the level of bilirubin needs phototherapy, one should pay attention to the treatment. After the bilirubin level is reduced, physicians have to make decisions on the moment of safe bilirubin cessation before risks such as bilirubin toxicity occur. Monitoring helps to make sure that the health of the baby will not be compromised.
The cancellation of phototherapy regimens must be considered in terms of serum bilirubin levels. Bilirubin clearance rate is also important and the clinical guidelines for jaundice should be followed to decide when treatment is safe to be discontinued.
Signs for Stopping Phototherapy Without Risk
A cessation of phototherapy may be safely achieved in situations where the bilirubin levels have decreased to below the phototherapy threshold. Physicians need to monitor the state of the baby and determine whether the level of bilirubin clearance is constant. Such improvement signs as the decrease of jaundice suggest that it is safe to cease the treatment. This phase depends on a clear understanding of whether the bilirubin level is phototherapy anymore.
When bilirubin levels stabilize over time, and the baby presents no evidence of bilirubin related damage to the brain, phototherapy can be withdrawn. This is so that there are no persistent threats to the health of the baby.
Monitoring During Phototherapy: What Parents and Doctors Must Know
It is important to regularly monitor serum bilirubin to monitor the effectiveness of the blue light phototherapy. To determine the success of the treatment, doctors examine the interpretation of the bilirubin chart. The parents are supposed to remain aware of the assessment of the severity of jaundice in the baby and abide by the instructions on prevention phototherapy.
In pregnant individuals with high risk newborns, including premature babies or babies with hemolytic disease, more frequent monitoring is required. It assists in the prevention of bilirubin toxicity and ensures that the baby is following the right path to recovery.
Next Steps if Phototherapy Alone is Not Enough
In case bilirubin does not reduce with blue light phototherapy, the alternative option is to contemplate exchange transfusion. This is accomplished when a significant toxicity of bilirubin is of concern, particularly during neonatal hyperbilirubinemia. Babies not responsive to phototherapy only may also need neonatal intensive care.
In this case, the doctors will also examine the amount of albumin and jaundice in the baby so as to come up with the most appropriate course of action. The condition of high bilirubin levels should be treated early enough to avoid kernicterus and brain damage caused by bilirubin.
FAQ’s
How high does bilirubin have to be to need phototherapy?
The bilirubin level must be above 15 mg/dL in full term babies, but lower levels are used with premature babies.
What is the normal range of phototherapy light?
The normal phototherapy range of light is approximately 460 to 490 nanometers, and this assists in dissolving bilirubin in the baby’s skin.
What should parents expect during phototherapy?
The parents may anticipate that their baby will be exposed to special light, and their eyes will be covered to protect them, and routine bilirubin level monitoring.
What is a toxic bilirubin level in a newborn?
The normal toxic bilirubin level is normally above 20 mg/dL and this could damage the brain when it is not remedied promptly.
What level of bilirubin causes brain damage in newborns?
An increase in bilirubin beyond 25 mg/dL may result in kernicterus, which is a form of brain damage in newborns.
Conclusion
Understanding the bilirubin level is phototherapy required is important in the control of neonatal jaundice. Early treatment using phototherapy will avoid severe complications, including brain injury due to bilirubin and kernicterus. Routine evaluation of bilirubin levels will make sure that the treatment process is initiated at the appropriate time and terminated without incidents. In full term and preterm infants, the awareness of the threshold of phototherapy and adherence to clinical recommendations on jaundice will ensure the safety of your baby. It is best to always consult the healthcare professionals in order to give your newborn the best care and results. A clear understanding of when a bilirubin level is phototherapy will support more effective and safer outcomes.